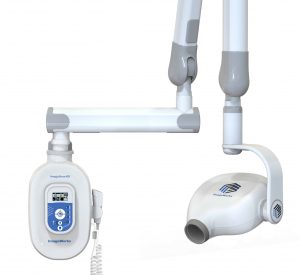
 Whether you are installing a dental intraoral x-ray in a new office, or you need to replace an old unit, it’s helpful to go into the process eyes wide open. In many cases, the questions below can be answered by the company providing your dental intraoral x-ray. However, it helps to understand all the requirements so that there are no surprises that cause delays or additional costs.
Whether you are installing a dental intraoral x-ray in a new office, or you need to replace an old unit, it’s helpful to go into the process eyes wide open. In many cases, the questions below can be answered by the company providing your dental intraoral x-ray. However, it helps to understand all the requirements so that there are no surprises that cause delays or additional costs. 1. Does it matter whether it’s a DC or AC x-ray? To answer this, it’s worth a quick explanation of the fundamental difference between a DC x-ray and an AC x-ray. Both types of wall mounted intraoral x-rays in a dental office (whether it is a DC x-ray or an AC x-ray) are powered by basic AC electricity that comes from the wall. The difference between a DC x-ray and an AC x-ray lies in what they do with that incoming electricity.
The incoming AC electricity is like a sine wave: it has pulses that go up and down. The power level (or intensity) of the x-ray generated by an AC x-ray matches this sine wave shape, and the actual x-ray power coming out of the machine oscillates at 60 times per second – like the input electricity.
A DC dental intraoral x-ray changes this input electricity so that the x-ray coming out of the unit is a single pulse that maintains more of a consistent power level through the entire exposure.
This difference in the profile of the x-ray output results in two subtle effects.
First, the “up and down” nature of the AC x-ray output creates more radiation when all other parameters are equal. Every time the power level is below a certain threshold, it is emitting radiation that is not having an impact on image quality (some refer to this as “soft radiation”). In other words, there is a small dose to the patient, but because it is below the sensitivity threshold of the film or sensor that’s capturing the image, it has no impact on the image. For AC x-ray, the power level is dipping below this threshhold 60 times per second, and therefore is emitting more of this soft radiation than a DC intraoral x-ray.
Second, there may be less consistent image quality when all other parameters are equal. If your exposure is 0.04 seconds in duration (not an uncommon setting), that’s only 2.5 “pulses” with an AC x-ray (because they occur 60 times per second). However, depending on the exact timing, the reality of that particular exposure could be 3 “peaks” and 2 “valleys”, or could be the other way around. This difference can create a slight inconsistency in the amount of exposure the sensor or film actually receives. In other words, two exposures taken with exactly the same parameters may have slightly different levels of energy applied to the sensor for an AC x-ray.
You may ask: why would anyone buy an AC x-ray? The answer is two-fold. First, there may be a price advantage with the AC x-ray. Second, the differences in both dosage and radiation are very slight, and both of these results are well within the federal requirements for these pieces of equipment.
2. Do I need a different dental intraoral x-ray if I am using film instead of digital sensors? The short answer is: typically no.
Typically, the amount of x-ray energy required to generate ideal images with film is higher than that required for a digital sensor. However, almost all intraoral x-ray units today have the ability to adjust settings. For most intraoral x-ray units, increasing the output power is done by simply switching the unit to a mode that increases the time (or duration) of the exposures (typically this is shown in milliseconds, or ms).
As an aside, if you are using film, the ideal parameters would also vary depending on which type of film you use (D speed, E speed, F speed, etc). Film speeds labelled as “slower” (like D-speed) require more energy to create the image than “faster” film speeds (like F-speed).
3. What shielding is required in the office? The official requirements will vary by state (and in some cases, by locality). However, here are some guidelines to consider.
The two most common characteristics of the office that are typically specified as requirements for intraoral x-ray operation are distance and wall material (sometimes referred to as “distance and density”). The reason for this is that these are two very effective protections against radiation.
Sometimes simply having 6 feet spacing between the intraoral x-ray and an operator is sufficient and no walls are required. Sometimes, a basic wall (typically referred to as “drywall” or “gypsum”) is required to separate the x-ray and the operator. Typically, most states will have some variation of these requirements. Rarely are lead-lined walls required for intraoral x-rays in dental offices. However, some state may require this if there is a very high volume of exposures being taken.
4. Can I have my repair person install my intraoral x-ray? Most states require that the intraoral x-ray be installed by a person who has registered with the state as a qualified installer. Therefore, if your repair guy has registered, then: “yes”. Otherwise, you want to make sure you are using a certified installer.
One of the ways the FDA monitors this is through a form that is filled out by the installer called the FDA 2579 form. The installer is required to complete this form, and then send one copy to the FDA and one copy to the state. A third copy is provided to the office, which is responsible for keeping a copy of this form to document that the piece of equipment was properly installed. It’s important to keep your copy, because it is common in many states that an inspector will come to the office periodically asking to see this document for each x-ray unit.
5. Do I need a wall-mounted unit, a mobile unit, or a handheld unit? This is a fundamental question that depends on your office needs. Handheld and mobile x-rays offer some economies of scale as they can be shared between rooms. However, there are performance aspects of a wall-mounted and a mobile unit that are often preferable to a handheld x-ray. For more on this question, see our post sharing more detail on these tradeoffs:
The Most Overlooked Pitfall of a Handheld X-Ray That Can Cost Your Practice Money
The intraoral dental x-ray is a critical component to a busy dental practice. Understanding some of key components involved in having a new intraoral x-ray installed in your office will help your team make sure there are no surprises.
If you have any questions about this process, please give us a call to talk to one of our specialists.
Call: 914-592-6100
Email: custserv@imageworkscorporation.com
The intraoral dental x-ray is a critical component to a busy dental practice. Understanding some of key components involved in having a new intraoral x-ray installed in your office will help your team make sure there are no surprises.
If you have any questions about this process, please give us a call to talk to one of our specialists.
Call: 914-592-6100
Email: custserv@imageworkscorporation.com
Subscribe to Receive More Great Articles
